
ICSI Treatment in Firozabad — Advanced Solution for Male Infertility
When a couple has been trying to conceive for a long time without success, the conversation almost always starts with the woman. Tests, scans, medications — the female partner often goes through months of investigations before anyone properly looks at the male side. And that is a problem, because in nearly half of all infertility cases, sperm quality or quantity plays a role.
ICSI — Intracytoplasmic Sperm Injection — was developed specifically to address that gap. It is one of the most significant advances in fertility medicine over the last three decades, and it has helped millions of couples worldwide have biological children despite severe male infertility. At Mittal Nursing Home & IVF Centre in Firozabad, ICSI is offered as part of a full range of assisted reproductive services under the care of Dr. Pratibha Mittal, a reproductive medicine specialist with advanced training in IVF and fertility surgery.
If you have been told that sperm-related issues are affecting your chances of conception — or if previous fertility treatments have not worked — this page is worth reading in full.

ICSI Treatment in Firozabad — Advanced Solution for Male Infertility
ICSI is a specialised form of IVF. The overall process — stimulating the ovaries, retrieving eggs, culturing embryos, and transferring them to the uterus — is exactly the same. The difference lies in one specific step: how the egg is fertilised.
In a standard IVF cycle, thousands of sperm are placed in a laboratory dish alongside the retrieved eggs. The sperm compete, and eventually one makes it through the egg’s outer layer and fertilises it. It is still a natural selection process, just happening outside the body rather than inside the fallopian tube.
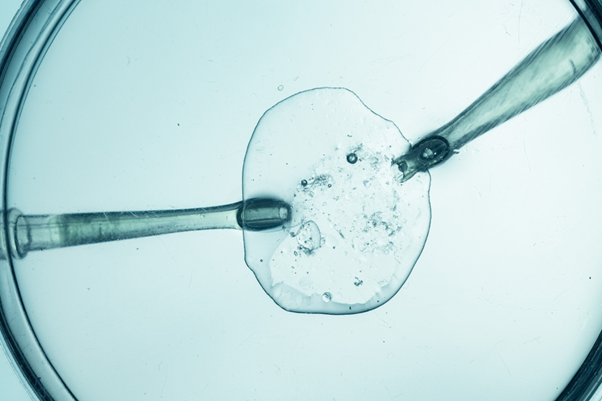
ICSI removes that competition entirely. A single sperm — hand-picked by a trained embryologist under a high-powered microscope — is drawn into an ultra-fine glass needle and injected directly into the centre of the egg. One sperm. One egg. No swimming, no competition, no chance of failure at the fertilisation stage due to poor sperm movement or penetration.
This makes ICSI enormously useful when the sperm simply cannot do that work on their own — whether because there are too few of them, they move too slowly, or their shape prevents them from penetrating the egg.
ICSI does not change the pregnancy success rate of IVF in cases where sperm quality is normal. It is specifically designed for — and most beneficial in — cases where male infertility is part of the picture.
Who Should Consider ICSI Treatment?
ICSI is not the right treatment for every couple facing infertility. It is specifically recommended when investigations point to a significant sperm-related factor. The most common situations where ICSI becomes the treatment of choice are:
Very low sperm count (oligospermia)
too few sperm in the ejaculate to rely on conventional fertilisation even in a lab setting.
Poor sperm motility (asthenospermia)
sperm that are present but cannot swim well enough to reach and penetrate an egg.
Abnormal sperm morphology (teratospermia)
an unusually high percentage of sperm with structural defects affecting fertilisation ability.
Complete absence of sperm in semen (azoospermia)
where sperm is either absent due to a blockage or not being produced in sufficient numbers. In these cases, sperm is surgically retrieved from the testes through TESA or PESA and used for ICSI.
Previous IVF cycle with failed or poor fertilisation
when eggs and sperm were placed together but fertilisation did not occur as expected.
Antisperm antibodies
where the body’s immune response interferes with sperm function.
Unexplained infertility after failed IUI cycles
ICSI is sometimes recommended as a more targeted next step.
ICSI Treatment in Firozabad — Advanced Solution for Male Infertility
Worth noting: ICSI does not require large numbers of sperm. Even men with extremely severe infertility — or those who have previously had a vasectomy — can potentially father a biological child through ICSI, as long as even a small number of viable sperm can be retrieved from the body.
Not sure if ICSI is the right treatment for you?
Get a complete male and female fertility evaluation at Mittal Nursing Home & IVF Centre, Firozabad. Dr. Pratibha Mittal will review your case and give you a clear, honest treatment recommendation — no unnecessary tests, no vague answers.
The ICSI Treatment Process — Step by Step
Knowing what to expect at each stage makes the process far less daunting. Here is how an ICSI cycle unfolds at Mittal Nursing Home & IVF Centre:
Step 1 — Complete Fertility Workup
Both partners are evaluated before anything begins. For the female partner: hormonal blood tests (FSH, LH, AMH, thyroid), a transvaginal ultrasound to check ovarian reserve and uterine structure, and sometimes a hysteroscopy if indicated. For the male partner: a detailed semen analysis covering count, motility, morphology, and in some cases sperm DNA fragmentation. This baseline is essential — treatment without proper diagnosis is guesswork.
Step 2 — Ovarian Stimulation
The female partner receives hormonal injections over roughly 10 to 14 days to encourage the ovaries to produce multiple mature eggs rather than the usual one. Monitoring scans are done at regular intervals to track follicle growth, and medication doses are adjusted based on how the ovaries respond.
Step 3 — Egg Retrieval.
Once the follicles reach the right size, eggs are collected in a brief procedure performed under conscious sedation. It usually takes 20 to 30 minutes. There is no general anaesthesia involved, and patients go home the same day.
Step 4 — Sperm Collection or Surgical Retrieval
On the day of egg retrieval, a semen sample is collected from the male partner. If there is no sperm in the ejaculate — azoospermia — sperm is retrieved directly from the testicular tissue through TESA (Testicular Sperm Aspiration) or from the epididymis through PESA, under local anaesthesia.
Step 5 — The ICSI Procedure
The embryologist selects the best-quality sperm from the sample and injects one into each mature egg individually, using a microscopic glass needle. This is done for every egg retrieved. The process requires considerable precision and skill — the quality of embryology work at this stage has a direct impact on fertilisation outcomes.
Step 6 — Embryo Culture and Monitoring
After fertilisation, embryos are kept in a controlled laboratory environment for three to five days. The embryologist monitors their development daily. Grading is done to identify which embryos have developed well enough to be considered for transfer.
Step 7 — Embryo Transfer
The best available embryo is transferred into the uterus using a thin, flexible catheter. It is a painless procedure, takes only a few minutes, and requires no anaesthesia. Any remaining good-quality embryos can be frozen for use in a future cycle.
Step 8 — Pregnancy Test
Fourteen days after embryo transfer, a blood beta-HCG test is done to check for pregnancy. Blood tests are more accurate at this stage than home kits, particularly given the hormonal medications taken during the cycle.
Is ICSI Safe? — What Research Says
This is a question that comes up in almost every ICSI consultation, and it deserves a straight answer rather than a reassuring non-answer. ICSI has been in use since 1992. In the three decades since, it has been studied extensively — and the overall picture is reassuring, though with some nuance worth understanding.
For the mother, the risks associated with ICSI are the same as those for standard IVF. The most significant concern is ovarian hyperstimulation syndrome (OHSS) — a condition where the ovaries over-respond to stimulation medications, causing swelling and discomfort. Mild OHSS is relatively common and resolves on its own. Severe OHSS is rare and is managed by adjusting stimulation protocols — experienced fertility specialists monitor for it closely throughout the cycle.
For children born through ICSI, the evidence is broadly reassuring. Large studies — including long-term follow-up data from Europe — have found that children conceived via ICSI develop normally and have health outcomes comparable to naturally conceived children in most measures. Birth defects occur at slightly higher rates in IVF and ICSI pregnancies compared to natural conception, but the absolute difference is small, and much of it is attributed to underlying factors in the parents rather than the procedure itself.
There is one area that requires honest discussion. Male infertility can sometimes have a genetic basis — certain chromosome abnormalities or gene deletions (such as Y-chromosome microdeletions) that affect sperm production. In some cases, these genetic factors can be passed on to sons conceived through ICSI. This does not mean ICSI should be avoided, but it does mean that genetic counselling and testing — such as karyotyping or Y-chromosome analysis — are worth discussing before treatment in cases of severe male infertility.
The bottom line from research: ICSI is a well-established, extensively studied procedure with a strong safety profile. For couples where male infertility is the obstacle, the benefits clearly outweigh the small additional risks — particularly when treatment is carried out by an experienced team in a well-equipped centre.
Research Note
A large-scale study published in Human Reproduction found no significant difference in cognitive development, motor skills, or overall health between children conceived through ICSI and those conceived naturally at age 5. Long-term follow-up studies from Belgium — where ICSI was first developed — have reached similar conclusions over 30 years of data.
Male Infertility and ICSI — Breaking the Silence

In many households across Firozabad and the wider region, infertility is still treated as a woman’s problem. The pressure falls on the wife — to be tested, to be treated, to explain. The husband’s fertility often goes unexamined for months or even years. This is both medically and emotionally costly.
The numbers tell a different story. In about 40 to 50 percent of infertile couples, a male factor is either the primary cause or a contributing one. A semen analysis — a straightforward, non-invasive test — can identify this in a matter of days. Yet many couples arrive at a fertility clinic after years of focus on the female partner, only to discover that the answer was on the other side all along.

This is not about blame. Sperm count, motility, and morphology issues are medical conditions — influenced by genetics, lifestyle, heat exposure, infections, hormonal factors, and in some cases unknown causes. They are no more a reflection of a man’s character or worth than a thyroid condition or a vitamin deficiency would be.
What matters is getting the right diagnosis early. At Mittal Nursing Home & IVF Centre, both partners are evaluated from the very first consultation. Because treating half the picture rarely gives you the full answer — and time, in fertility treatment, is something you genuinely cannot afford to waste.
Why Choose Mittal Nursing Home & IVF Centre for ICSI in Firozabad?

Until a few years ago, couples in Firozabad who needed ICSI had no real choice but to travel — to Agra, to Delhi, sometimes further. The cost, the logistics, the stress of managing a fertility cycle far from home. All of that is no longer necessary.
Mittal Nursing Home & IVF Centre now offers a fully equipped ICSI programme within Firozabad. The centre has an in-house embryology laboratory, a dedicated IVF unit, and an operating theatre for egg retrieval and surgical sperm retrieval procedures. Everything needed for a complete ICSI cycle is available under one roof.
Dr. Pratibha Mittal brings an unusual combination of qualifications to this work. Her MS in Obstetrics and Gynaecology from Maulana Azad Medical College, New Delhi was followed by a Fellowship in Reproductive Medicine from Fortis Hospital, Shalimar Bagh — one of India’s leading tertiary fertility centres. She also holds MRCOG Part I from the Royal College of Obstetricians and Gynaecologists, UK. Outside of metro cities, that level of training is rare.

The centre is also home to Firozabad’s first laparoscopy and hysteroscopy facility — which means that if a surgical correction to the uterus or fallopian tubes is needed alongside fertility treatment, it can be done here. No referrals elsewhere. No splitting your care between different doctors and different cities.
And practically speaking — patients are seen and managed directly by Dr. Mittal throughout their cycle. Monitoring appointments, protocol adjustments, the transfer itself. You are not passed between a consultant and a team of rotating junior doctors. That continuity of care makes a difference, particularly during a process as emotionally and medically intensive as ICSI.
What to Expect After Embryo Transfer in an ICSI Cycle
The two weeks between embryo transfer and the pregnancy blood test are almost universally described as the hardest part of the ICSI journey. The medical intervention is over. There is nothing left to do but wait. And for couples who have been through months or years of trying, that wait carries an enormous amount of hope — and fear.
A few practical points for this period. Continue all prescribed medications — particularly progesterone support — exactly as directed. Do not stop or reduce them without checking with the clinic first, even if you feel fine. Light activity and normal daily life are generally fine after the first day or two of rest following transfer. Strenuous exercise, heavy lifting, and situations of significant physical or emotional stress are better avoided — not because they directly affect implantation, but because rest is genuinely good for you at this stage.

Avoid taking a home pregnancy test before Day 14. The hormonal medications used in IVF and ICSI cycles — particularly HCG trigger injections — can produce a false positive result on a urine test for several days after transfer. A blood beta-HCG test at the clinic on Day 14 gives a clear, reliable result.
Contact the clinic promptly if you experience significant pelvic pain, heavy bleeding, or fever. Mild spotting in the days after transfer is not uncommon and is not necessarily a sign that the cycle has failed — but any symptoms that concern you should be reported rather than waited out at home.
Whatever the result on Day 14, Dr. Pratibha Mitthal, one of the best IVF doctor in Firozabad will discuss the next steps with you in full. A positive result marks the beginning of early pregnancy monitoring. A negative result — while deeply disappointing — is the start of a conversation about what comes next, not the end of the road.
Mittal Nursing Home & IVF Centre offers complete ICSI treatment in Firozabad — from semen analysis and fertility workup to embryo transfer and pregnancy follow-up. Take the first step today.
ICSI Treatment in Firozabad — Advanced Solution for Male Infertility

ICSI achieves fertilisation in approximately 70 to 85 percent of injected eggs on average — a significantly better result than conventional IVF in cases where sperm quality is poor. But fertilisation is only one part of the picture. Whether a fertilised egg develops into a healthy embryo, implants successfully, and results in a live birth depends on several additional factors.
The woman’s age is one of the most significant variables. Under 35, pregnancy rates per cycle are generally higher. Between 35 and 40, they begin to decline — though they remain reasonable with good ovarian response and quality embryos. Above 40, success rates are lower, but cases vary considerably depending on individual circumstances.
Embryo quality matters a great deal. Two couples can have similar sperm profiles but very different embryo development — and that difference shapes the outcome. Ovarian reserve, uterine receptivity, and overall health all play a role too.

Dr. Pratibha Mittal, one of the best IVF doctor in firozabad has maintained consistently strong success rates across IVF and ICSI cycles, having performed the highest number of assisted reproductive cycles in the region. Every patient is given a personalised success estimate during consultation — based on their actual test results, not a generalised figure pulled from a brochure.
FAQs
Is the ICSI procedure painful for the male partner?
For most men, sperm collection is straightforward and non-invasive. In cases requiring surgical sperm retrieval — TESA or PESA — the procedure is done under local anaesthesia and is generally described as mild discomfort rather than significant pain. Recovery is quick, usually within a day.
Does ICSI guarantee that fertilisation will happen?
No fertility treatment can offer a guarantee. ICSI achieves fertilisation in approximately 70 to 85 percent of injected eggs — a high rate, but not 100 percent. Not every fertilised egg develops into a viable embryo, and not every embryo transfer results in pregnancy. Your doctor will walk you through realistic expectations based on your specific results.
Are babies born through ICSI healthy?
Research consistently shows that children born through ICSI are healthy and develop normally. There is a small increase in the rate of certain chromosomal conditions compared to natural conception, but this is largely associated with the underlying male infertility rather than the procedure itself. Your fertility specialist will discuss any specific genetic considerations relevant to your case before treatment begins.
What happens to embryos that are not transferred?
Good-quality embryos that are not used in the fresh transfer can be frozen (vitrified) and stored for future use. Frozen embryo transfer (FET) cycles are simpler, less medication-intensive, and often have comparable success rates to fresh transfers — making them a valuable option if the first cycle does not succeed or if the couple wants another child later.
How many ICSI cycles might be needed?
Many couples succeed on the first or second cycle. The number of cycles recommended depends on your age, diagnosis, embryo quality, and how the ovaries responded to stimulation. If frozen embryos are available from the first retrieval, subsequent cycles are less intensive and less expensive. Your doctor will outline a realistic plan with you after reviewing your full workup.
Can ICSI be done if there is zero sperm in the semen?
In many cases, yes. If sperm is absent from the ejaculate due to a blockage — rather than a complete absence of sperm production — it can often be retrieved directly from the testes or epididymis through TESA or PESA and used for ICSI. An evaluation will determine whether surgical retrieval is possible and what the likely outcomes are.

 English
English
 हिंदी
हिंदी